Global health’s workforce crisis is usually framed as a shortage problem. That frame is too narrow. The deeper crisis lies in how health systems depend on women’s labor while continuing to undervalue, underprotect, and underrepresent the workers on whom care depends.
A workforce crisis built on invisible assumptions
Global health has a workforce problem. Governments, multilaterals, and health leaders warn of shortages, burnout, migration pressures, and weak retention. The World Health Organization estimates that the world will still face a shortfall of 11 million health workers by 2030, concentrated largely in low- and lower-middle-income countries. That figure matters, but the standard framing makes the crisis sound more technical than it is. It suggests a problem of supply and planning, when the deeper issue is the labor model on which many health systems already depend.
The crisis is not only about how many workers are available. It is also about who performs the work, how that work is valued, and which forms of labor institutions have learned to treat as endlessly stretchable. WHO reported in 2024 that women make up 67% of the paid global health and care workforce and perform 76% of unpaid care work worldwide. Those figures should change how the shortage debate is understood. Health systems are relying on labor performed largely by women while continuing to underpay, underprotect, and structurally discount the work on which care depends.
That arrangement has consequences. A sector built around labor that is moralized rather than properly valued will predictably struggle with retention, burnout, and weak workforce stability. WHO’s 2024 analysis was explicit: work done primarily by women tends to be paid less and carried out in poorer working conditions, with broader effects on wages, productivity, and the strength of the sector itself.
Health systems are relying on labour performed largely by women while continuing to underpay, underprotect, and structurally discount the work on which care depends.
Women deliver care. Men still dominate power
The imbalance is visible across the occupations that keep health systems functioning every day. Nursing, midwifery, caregiving, and much of frontline service delivery remain heavily feminized. These are not peripheral functions. They involve clinical judgment, continuity of care, patient education, emotional discipline, and the daily management of risk in overstretched institutions. Yet they are still too often treated as support work rather than system-defining work. That distinction shapes pay, status, staffing, and whose concerns are treated as operationally central.
The hierarchy becomes even clearer at the top. WHO’s gender and leadership analysis found that women make up almost 70% of the global health and social workforce but hold only 25% of senior roles. This is often discussed as a representation gap. It is more consequential than that. Leadership determines budgets, staffing models, promotion structures, and the degree of seriousness attached to workplace safety, flexibility, and retention. When the people delivering most of the care remain underrepresented in decision-making, the burdens they carry are easier for institutions to normalize.
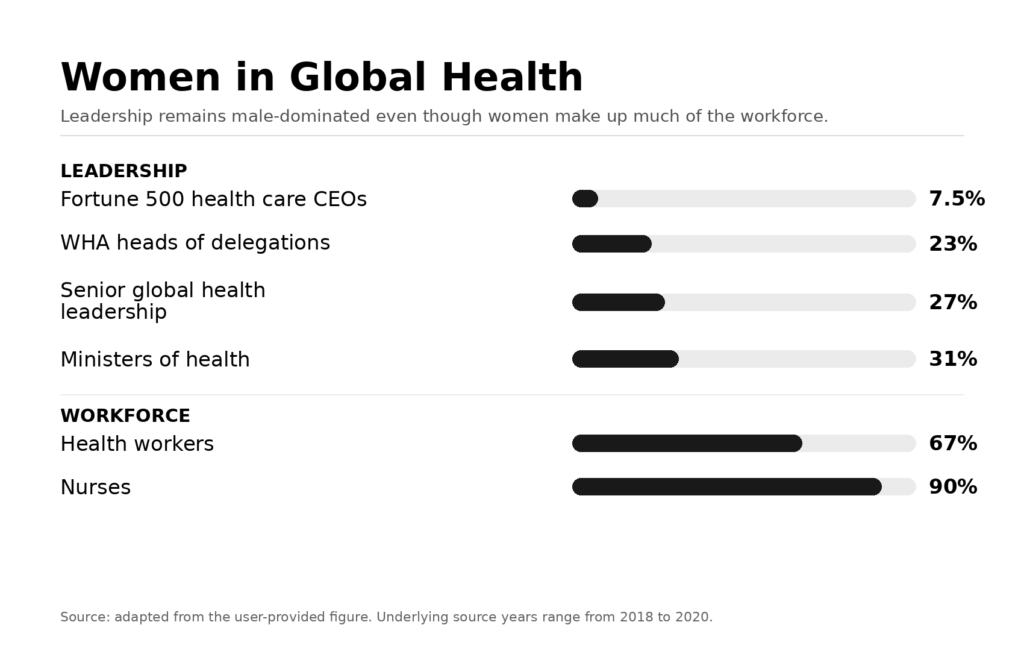
The result is a familiar contradiction: women are essential to the functioning of health systems, but remain less influential in setting the terms on which that work is done. Flexible scheduling, progression after maternity, supportive supervision, and protection from workplace violence are then treated as secondary concerns rather than workforce fundamentals.
The pay gap is not incidental
Pay exposes the same structure more clearly. The International Labor Organization and the WHO reported that women in the health and care sector earn 24% less than men on average, a wider gender pay gap than in the broader economy. Their joint analysis also found that part of that gap remains unexplained by occupation or working time, pointing to structural discrimination rather than simple differences in role or hours worked.
A sector that underpays the majority of its workforce weakens its own recruitment and retention pipeline.
This matters for reasons beyond fairness. A sector that underpays the majority of its workforce weakens its own recruitment and retention pipeline. It also signals that certain forms of expertise can be relied upon without proper compensation. Public praise for care work does not offset chronic financial undervaluation. Where pay remains persistently weak, institutions eventually pay in other ways: vacancy, attrition, burnout, and avoidable instability.
The same logic extends beyond wages. Women do not enter the health workforce from a neutral starting point. WHO estimates that women perform 76% of unpaid care work. This is part of the labor infrastructure on which formal health systems depend. Workers are expected to sustain paid care inside institutions while continuing to absorb childcare, eldercare, and domestic labor outside them. That affects who can train, who can work nights, who can relocate, and who leaves when the burden becomes unsustainable.
Flexible scheduling, safe staffing, career progression after maternity, protection from workplace violence, and investment in supportive supervision are then treated as secondary matters rather than operational priorities. The result is a familiar contradiction: women are essential to the functioning of health systems, but they remain less influential in defining the terms on which that work is done.
Migration redistributes scarcity
Migration reveals another fault line. High-income countries with aging populations and domestic staffing gaps often respond by recruiting nurses and other health workers from abroad. That may ease pressure in destination countries, but it can deepen scarcity in places already struggling with weaker health systems and lower fiscal capacity. WHO notes that one in eight nurses practices in a country other than the one where they were born or trained, while its broader workforce analysis continues to locate the largest projected shortages in lower-income settings.
Mobility can create opportunities for individual workers, and that should be acknowledged. But the broader pattern remains difficult to defend. Richer systems can delay politically harder reforms on pay, training, and working conditions by drawing on labor educated elsewhere. Poorer systems lose experienced staff and are then told to do more with fewer resources. Migration, in this sense, does not solve the workforce crisis. It redistributes it through a labor market that rewards purchasing power more than health needs.
Care labor must be treated as infrastructure
The deeper problem is that global health still struggles to treat care labor as core infrastructure. Medicines, buildings, digital systems, and supply chains are readily understood as investments. Care work is still too often handled as a cost center or a vocation sustained by sacrifice. That distinction shapes policy. When care is romanticized, underpayment becomes easier to justify. When exhaustion is normalized, retention failure starts to look inevitable rather than produced.
A more serious response would begin with valuation. Equal pay and pay transparency should be fundamental to the workforce. Retention should be addressed through safer staffing, secure contracts, stronger career ladders, and protection from workplace violence. Leadership reform should focus on appointments, authority, and accountability. International recruitment should adhere to ethical standards, while high-income countries invest more seriously in domestic training and retention. WHO and ILO’s work makes clear that working conditions and pay equity are not peripheral social issues. They are central to workforce performance.
The global health workforce crisis is real. It is also gendered at its core. Any response that counts workers without changing the labor model will leave the basic structure intact. The likely result is familiar: more recruitment drives, more praise for frontline staff, and the same quiet assumption that women’s labor will stretch a little further.















