Career advice in public health often begins in the wrong place.
Professionals describe the feeling in similar terms: overwhelmed, misaligned, uncertain where they belong. The guidance they receive is usually well-meaning: find your niche, build your brand, gain more experience, become more strategic.
That advice may help at the margins, but it misreads the problem.
The confusion is often treated as an individual deficit. In many cases, it is better understood as a structural feature of the field itself.
Public health is presented as a single profession. In practice, it functions as a set of connected worlds, each with its own pace, authority structure, evidence standard, and definition of impact.
The World Health Organization’s work on essential public health functions makes this breadth explicit: workforce strengthening requires countries to define public health services, map the range of occupations involved, and align competencies with employment and public health needs. That is a workforce architecture problem, not merely a career-planning problem.
Much of the uncertainty public health professionals experience comes from entering a field that asks them to move across communities, institutions, evidence systems, emergency settings, policy processes, and care environments without first teaching them how those spaces differ.
The Field Contains Competing Operating Systems
Public health is broad by design. It includes disease prevention, health promotion, policy, surveillance, emergency response, communication, equity work, service delivery, and systems reform. The 10 Essential Public Health Services, widely used in the United States, describe public health activity across assessment, investigation, communication, community partnership, policy, regulation, access to care, workforce development, evaluation, and organizational infrastructure.
That breadth is a strength. It is also a source of professional ambiguity.
A person trained in epidemiology may struggle in community engagement work because the work is governed by a different standard of success. Epidemiology privileges measurement, inference, and reproducibility. Community engagement depends on trust, continuity, and legitimacy. A community health worker brought into a policy process may hit a wall because institutional decision-making often moves through budgets, mandates, legal authority, and procedural timelines that sit far from the pace of lived experience.
The field presents itself as coherent while functioning through distinct domains. That gap between presentation and practice is where much professional confusion lives.
The ambiguity is visible in the way the workforce itself is defined. A 2024 exploratory analysis of WHO policy and the literature found diverse understandings of the scope of the public health workforce across countries and settings, including macro-, meso-, and micro-level perspectives. Public health has shared population-health aims, but it does not have a single occupational center. Its work is carried out through different institutions, methods, accountabilities, and time horizons.
Six Interconnected Worlds
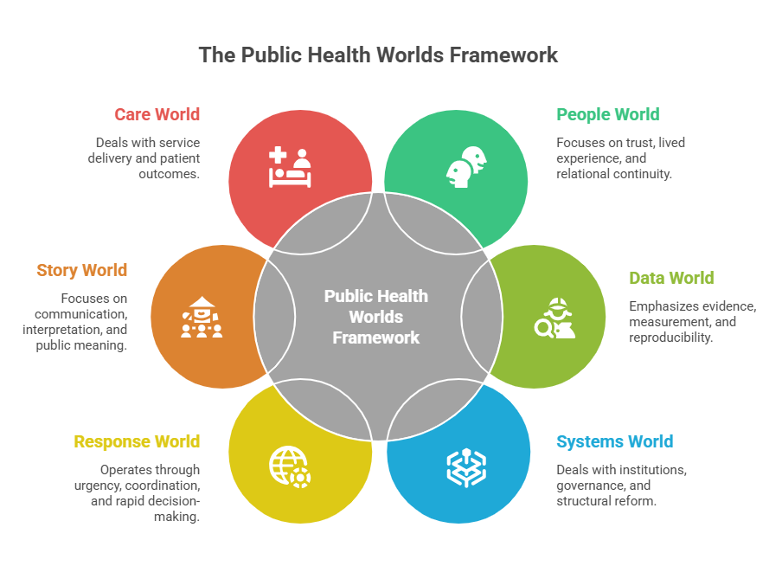
The Public Health Worlds Framework organizes the field into six interconnected worlds: People, Data, Systems, Response, Story, and Care.
The framework is about how work is organized, how decisions are made, and how impact is judged.
The People World prioritizes trust, lived experience, and relational continuity. Its timeline is long. Success depends on legitimacy sustained over time.
The Data World prioritizes evidence, measurement, and reproducibility. Its timeline is methodical and iterative. Success depends on findings that can withstand scrutiny.
The Systems World prioritizes governance, structure, financing, regulation, and institutional reform. Its timeline often stretches across years. Success depends on whether change can endure beyond a project cycle.
The Response World prioritizes speed, coordination, and rapid decision-making under uncertainty. Its timeline is immediate. Success depends on stabilization and containment.
The Story World prioritizes meaning, interpretation, and communication. Its timeline is adaptive. Success depends on whether information becomes understandable, credible, and socially resonant.
The Care World prioritizes delivery, operational continuity, and patient outcomes. Its timeline is continuous. Success depends on whether systems function reliably in practice.
These worlds overlap constantly. A vaccination campaign may require data systems, trusted community relationships, logistics, policy authority, clinical delivery, and public communication at the same time. The campaign may sit under one public health label while depending on several different ways of working.
When those differences remain unnamed, professionals often mistake structural friction for personal inadequacy.
Why Misalignment Feels Personal
Different public health worlds reward different professional instincts. Data rewards caution. Response rewards speed. People rewards trust. Systems rewards durability. Story rewards interpretation. Care rewards reliable delivery.
The tension between Data and Response shows the problem clearly. One waits for stronger evidence. The other acts before certainty exists because delay can carry its own harm. Each is trying to prevent a different failure: weak inference on one side, avoidable delay on the other.
The same tension appears between People and Systems. Community work often moves at the speed of trust. Institutions often move at the speed of process. One depends on relational accountability and local legitimacy. The other depends on consistency, compliance, scale, and durability.
These differences matter because professionals are often asked to move between worlds without being told that the rules have changed. Someone moving from emergency response into research may feel undisciplined. Someone moving from research into operations may feel slow. Someone moving from community engagement into institutional policy may feel distant from the populations they entered public health to serve.
The problem is often mismatch. A competent person can struggle when their training, instincts, and values are poorly aligned with the demands of a role, organization, or moment.
Individual advice is too thin for a field this complex.
The cost is not only personal frustration. Misalignment can weaken collaboration, distort performance expectations, and make capable professionals question whether they belong in a field that has not clearly explained its own internal rules.
What the Framework Changes
The Public Health Worlds Framework gives professionals a way to diagnose the structure of their work before diagnosing themselves.
Instead of asking only, “What job title should I pursue?” a professional can ask more useful questions:
Which world does my training most closely align with? Which world is my current institution actually operating in? What kind of decision-making comes naturally to me? Am I working in a setting that rewards that instinct or punishes it?
When the answers align, work tends to feel more coherent. Effort translates more visibly into impact. When they do not align, the professional has a structural explanation and a starting point for more deliberate movement.
The same diagnostic lens helps organizations.
A program built on Systems World assumptions but staffed mainly by Response World professionals may struggle because people are working from different definitions of progress. A community initiative evaluated mainly through Data World metrics may appear weak if its most important early gains involve trust, participation, or legitimacy. A care-delivery reform may fail if policy design ignores the operating realities of clinics, frontline staff, and patients.
Public health already recognizes the value of shared competencies. CDC describes the Core Competencies for Public Health Professionals as a framework for workforce development planning and action, rooted in the broad practice of public health and defined by the 10 Essential Public Health Services. Competency frameworks are necessary. They help define what professionals should know and be able to do.
Career coherence requires something more: structural literacy. Professionals need to understand which decision system a setting is using, where that system is useful, and where it creates blind spots.
The Field Needs Better Structural Literacy
Public health career coaching often asks people to clarify their interests. That remains useful. It is incomplete without a clearer account of the field’s internal architecture.
Students should leave public health education with more than a list of possible sectors. Early-career professionals should learn how roles differ in pace, power, accountability, evidence standards, and definitions of success. Hiring managers should be clearer about the world a role actually sits in, rather than relying on broad job descriptions that make every position sound equally strategic, collaborative, and impact-oriented.
Mentors should be able to distinguish between a professional who lacks preparation and one who is working in the wrong operating environment. Institutions should be able to see when poor collaboration reflects a mismatch in timelines, incentives, and decision rules rather than a failure of commitment.
Public health is not one path. It is a system of interconnected worlds. Professionals should not have to mistake the field’s complexity for their own confusion.
Public health is not one path. It is a system of interconnected worlds. Professionals deserve a better map, and they should not have to mistake the field’s complexity for their own confusion.
Dr. Sadia A. Sony is a public health consultant and global health specialist whose work focuses on health systems, workforce navigation, and the structural complexity of public health institutions. Her experience spans clinical care, public health programming, research, and community health across South Asia and Canada. She is the creator of the Public Health Worlds Framework.